Vulva - Tumoren: Therapie
Allgemeines
Operation
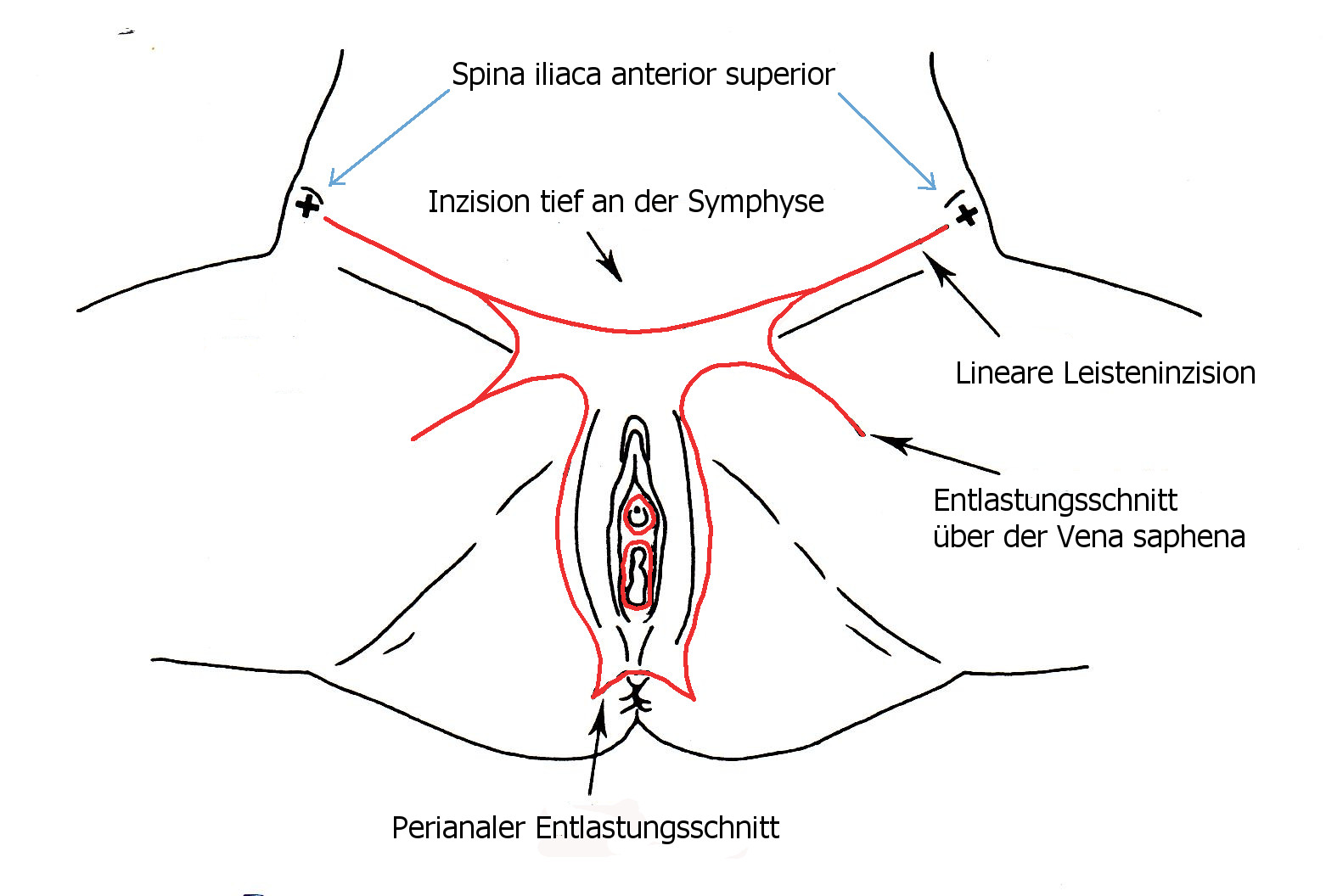
Wegen der häufigen Wundkomplikationen kaum noch angewendet.
Radiatio
Chemotherapie
Therapie der HPV-assoziierten VIN
offene Protokolle
Teil von
Quellen
1.) AGO
Interdisziplinäre S2k-Leitlinie für die Diagnostik und Therapie des Vulvakarzinoms und seiner Vorstufen.
Zuckschwerdt Verlag, München 2009
2.) Beriwal S, et al.:
Preoperative Intensity Modulated Radiation Therapy and Chemotherapy for Locally Advanced Vulvar Carcinoma: Analysis of
Pattern of Relapse.
Int J Radiation Oncol Biol Phys 2013;85:1269-1274
http://dx.doi.org/10.1016/j.ijrobp.2012.11.012
3.) Way S:
The anatomy of the lymphatic drainage of the vulva and its influence on the radical operation for carcinoma.
Ann R Coll Surg Eng 1948;3:187
4.) Way S:
Carcinoma of the vulva.
Am J Obstet Gynecol 1960;79:692-698
5.) Way S:
The surgery of vulval carcinoma:an appraisal.
Clin Obstet Gynecol 1978;5:627
